Getting a handle on your cholesterol is one of the most proactive steps you can take for your heart health. It's about striking the right balance between the 'good' and 'bad' types flowing through your blood. This balance is absolutely vital; your body genuinely needs cholesterol to build healthy cells and produce hormones, but when things get out of whack, it can quietly lead to serious problems down the road. This guide provides medically sound advice and practical tips to help you manage your levels through positive lifestyle changes.
So, What Is Cholesterol and Why Should I Care?
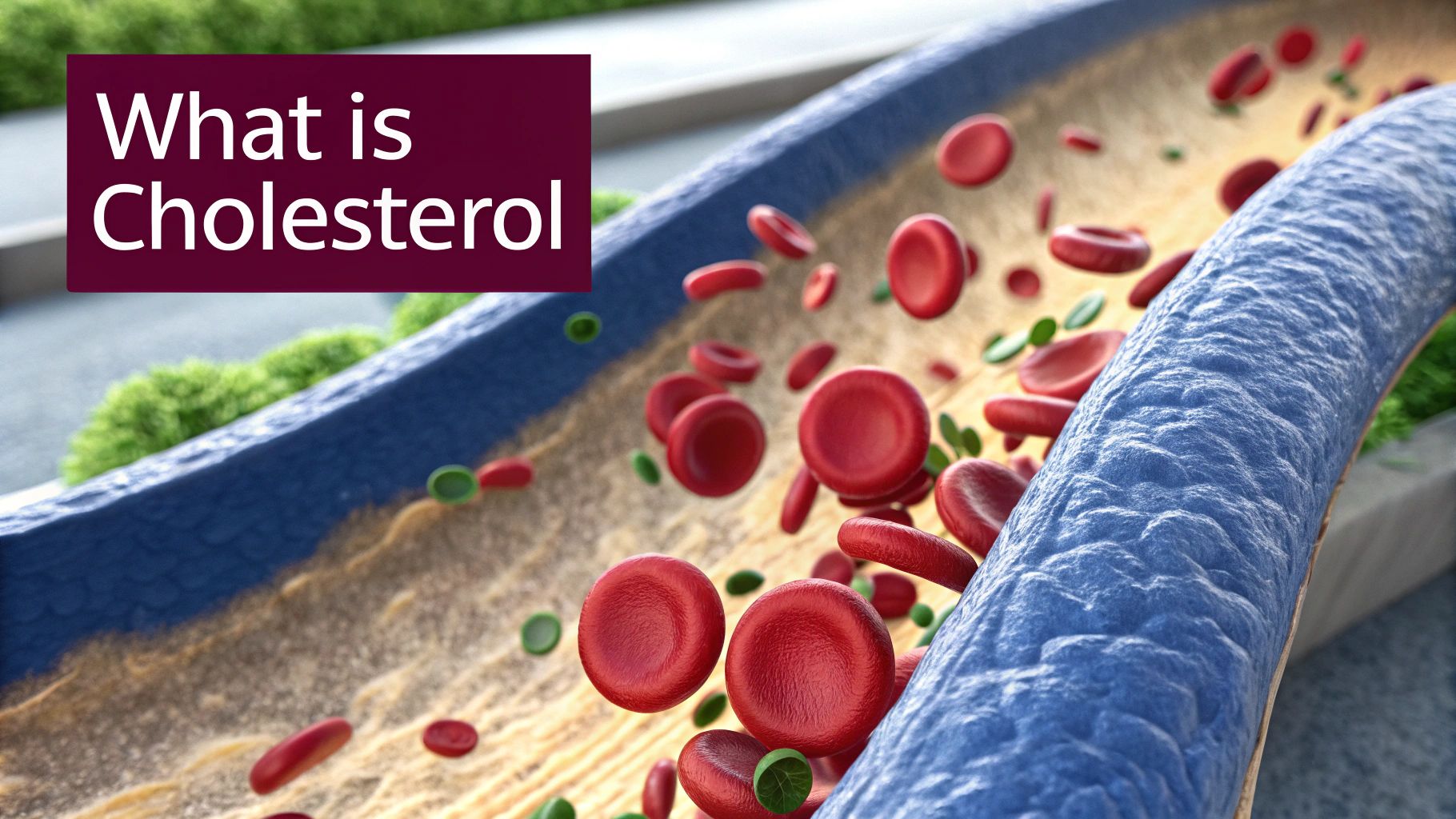
Cholesterol often gets a bad rap, but it’s essentially a waxy, fat-like substance that your body can't live without. Your liver actually makes all the cholesterol you need, but we also top it up through foods like meat, cheese, and eggs.
Here’s the thing: because cholesterol is a fat, it can't just dissolve and travel freely in your blood, which is mostly water. Think of oil and vinegar. To get around this, cholesterol hitches a ride on special protein escorts. These little bundles of fat and protein are called lipoproteins.
Getting to know these lipoproteins is the secret to understanding your cholesterol results. They are the vehicles that decide whether cholesterol is helping your body or silently clogging up your arteries.
The Delivery Trucks and The Cleanup Crew
When you look at your blood test, you'll see two main types of these lipoprotein vehicles. Each has a completely different job.
Low-Density Lipoprotein (LDL) is the one you’ve probably heard called ‘bad’ cholesterol. Think of LDL as a fleet of delivery trucks. Their job is to drop off cholesterol from your liver to all the cells that need it. This is a crucial service, but too many trucks on the road can cause chaos. If you have too much LDL, it starts depositing its cargo on the walls of your arteries, creating a hard, waxy buildup called plaque.
This buildup narrows your arteries and makes them stiff, a condition called atherosclerosis. Over time, these arterial traffic jams can choke off blood flow, dramatically increasing your risk of a heart attack or stroke.
High-Density Lipoprotein (HDL) is the ‘good’ cholesterol. If LDLs are the delivery trucks, then HDLs are the motorway’s cleanup crew. These particles cruise through your bloodstream, picking up stray, excess cholesterol from your arteries and hauling it back to the liver. Once there, the liver processes it and gets rid of it for good.
Health Tip: A higher HDL level is a great sign. It means you have an efficient cleanup system running, actively removing the gunk that could otherwise cause blockages. You can boost your HDL through regular aerobic exercise, like brisk walking, swimming, or cycling.
Other Key Players on Your Results Sheet
Your cholesterol test, often called a lipid panel, doesn't stop at just LDL and HDL. It gives you a more complete picture by measuring a few other things.
- Triglycerides: This is a different type of fat in your blood. When you eat, your body converts any extra calories it doesn’t need right away into triglycerides and stores them in your fat cells. Consistently high levels are often a sign of a diet high in sugar, refined carbohydrates, and alcohol.
- Non-HDL Cholesterol: This is a simple but really useful number your doctor looks at. It's your total cholesterol minus your HDL cholesterol. Essentially, it bundles all the 'bad' cholesterol types together into one figure and is now seen as one of the most accurate predictors of heart disease risk.
At the end of the day, it's not about one single number. It’s about the overall balance between all these moving parts. A healthy cholesterol profile means your body's delivery and maintenance systems are working in harmony, keeping everything running smoothly without causing dangerous backups.
Decoding Your UK Cholesterol Test Results
Getting your cholesterol test results back—often called a lipid panel—can feel a bit like trying to read a foreign language. You're faced with a page of acronyms and numbers, but don't worry. Learning what they mean is the first real step you can take towards protecting your heart health.
Think of it as a detailed report card on how your body is handling different fats. Your GP won’t just fixate on one number; they'll look at the whole picture. They piece together your results with other vital information, like your age, family history, and blood pressure, to get a clear idea of your personal risk. Knowing what these figures represent means you can have a much more productive chat with your doctor about lifestyle changes.
Understanding the Key Numbers in mmol/L
Here in the UK, we measure cholesterol in millimoles per litre (mmol/L). And it’s a big deal for public health. To give you some context, past data revealed that a staggering 56% of adults in Scotland had total cholesterol levels over the 5.0 mmol/L mark, which is considered 'raised'. It shows just how common this issue is.
To help you get to grips with your own report, let's break down what each measurement means and the ranges you should be aiming for.
UK Cholesterol and Triglyceride Reference Ranges
This table offers a clear guide to the typical reference ranges for cholesterol and triglycerides in the UK, measured in millimoles per litre (mmol/L). Use it to see where your numbers fall.
| Measurement | Healthy Level (mmol/L) | Borderline High (mmol/L) | High (mmol/L) |
|---|---|---|---|
| Total Cholesterol | 5.0 or below | 5.1 to 6.4 | 6.5 or above |
| LDL Cholesterol | 3.0 or below | 3.1 to 4.1 | 4.2 or above |
| Non-HDL Cholesterol | 4.0 or below | 4.1 to 5.1 | 5.2 or above |
| HDL Cholesterol | Above 1.0 (men) / 1.2 (women) | N/A | N/A (higher is better) |
| Triglycerides | 2.3 or below | 2.4 to 5.6 | 5.7 or above |
Remember, these are general guidelines. Your personal targets might be different based on your overall health profile, which is something your doctor will discuss with you.
This simple visual guide helps to put those main cholesterol markers into perspective.

As you can see, the aim of the game is to keep your LDL and Total Cholesterol down while making sure your HDL level is nice and high. It’s all about finding that healthy balance.
What Do These Results Mean for You?
So, you’ve got your numbers. What happens now? Your results are the perfect jumping-off point for a conversation about your lifestyle. If any of your figures creep into that borderline or high zone, it’s not a cause for panic. Instead, view it as a powerful motivation to adopt healthier habits.
These lifestyle tweaks are incredibly powerful tools for getting your numbers back on track:
- Smart Food Swaps: Cutting back on saturated fats (found in fatty meats, biscuits, and full-fat dairy) is key. At the same time, boost your intake of soluble fibre from foods like oats, apples, beans, and vegetables.
- Get Moving: Aim for at least 150 minutes of moderate activity a week. Something as simple as a brisk walk can make a real difference, especially in raising your protective HDL levels.
- Manage Your Weight: Even losing a small amount of excess weight can have a surprisingly big and positive effect on both your cholesterol and triglyceride levels.
Getting to know your results is a huge step. If you're keen to stay on top of your health, you might want to learn more about arranging a private blood test in the UK to keep an eye on things. At the end of the day, these results aren't just numbers on a page—they're your personal roadmap to a healthier heart.
How High Cholesterol Affects Your Heart Health
It’s one thing to see the numbers on your cholesterol report, but it’s another thing entirely to grasp what they mean for your heart. The connection is direct and powerful, and a simple analogy can help make sense of it all.
Think of your arteries as perfectly clean, smooth pipes carrying blood where it needs to go. Now, imagine excess LDL (‘bad’) cholesterol is a bit like sticky grease or limescale. When there’s too much of it floating around in your bloodstream, it starts to cling to the inside walls of those pipes.
This sneaky build-up of fatty deposits is a process known as atherosclerosis. Over many years, these deposits—called plaque—can grow and harden, making the arteries narrower and narrower. It's a slow, silent process that chokes off the space for blood to flow freely.
The Silent Narrowing of Your Arteries
As your arteries become constricted and stiff, your heart is forced to work much harder to push blood through the smaller openings. That strain alone isn't great, but the real danger comes from the plaque itself, which can become fragile and break open.
When a plaque ruptures, your body’s natural defence mechanism kicks in and forms a blood clot to repair the damage. The problem is, in an already narrowed artery, that clot can easily become a complete blockage, like a dam stopping a river.
The consequences are severe:
- If the blockage happens in an artery feeding the heart, it triggers a heart attack.
- If it cuts off blood flow to the brain, it causes a stroke.
This is exactly how high cholesterol becomes a major player in life-threatening cardiovascular events. It’s a process that usually flies under the radar, showing no symptoms until the situation is critical.
HDL Cholesterol: Your Protective Force
Thankfully, it's not all bad news. This is where HDL (‘good’) cholesterol comes into play. Think of HDL as your body’s own specialised cleaning crew.
HDL particles travel through your arteries, scouting for excess LDL cholesterol. They collect it and carry it back to the liver, where it's broken down and removed from your system for good.
Health Tip: Having healthy HDL levels is vital for protecting your heart. You can actively increase your HDL by engaging in regular physical activity, quitting smoking, and incorporating healthy monounsaturated fats (like those in olive oil and avocados) into your diet.
In the UK, high LDL cholesterol is a well-known and modifiable risk factor for heart disease. These are factors we have control over, and they contribute significantly to cardiovascular deaths here and across the globe. For a deeper dive into the worldwide impact, the British Heart Foundation has a detailed factsheet that breaks it down.
You Have the Power to Change Your Numbers
Getting your cholesterol results is one thing, but what comes next is where you really take control. While your genes do have a say, don't underestimate the power of your daily habits. Think of this as your practical guide to nudging those numbers in the right direction, one simple, sustainable step at a time.
This isn't about a massive, overnight life overhaul. It's about making small, smart swaps that, over time, add up to a big win for your heart.
Start With What's on Your Plate
The connection between what you eat and your cholesterol levels is direct and undeniable. The good news is that it’s less about strict deprivation and more about making clever choices that actively support your body’s health. The main goal is simple: cut back on saturated and trans fats and bring in more of the good stuff that helps clear out the bad.
Think of soluble fibre as a natural sponge. As it moves through your digestive system, it soaks up cholesterol and helps escort it out of your body before it can get into your bloodstream. It’s easy to get more of it into your diet:
- Oats and Barley: A warm bowl of porridge is more than just comfort food; it's a brilliant start to a heart-healthy day.
- Fruits: An apple a day really does help. Pears, oranges, and berries are also fantastic sources of soluble fibre.
- Legumes: Lentils, chickpeas, beans, and peas are true nutritional powerhouses.
At the same time, make friends with healthy fats. Omega-3 fatty acids, found in oily fish like salmon, mackerel, and sardines, are particularly great for lowering triglycerides and keeping your heart in good shape.
Health Tip: Remember this simple rule: eat more whole, unprocessed foods. They are naturally lower in the kinds of fats that raise LDL and packed with the fibre and nutrients you need to lower it. Aim for a colourful plate filled with fruits, vegetables, and whole grains.
To make this even easier, here are some simple swaps you can make in your daily routine.
Dietary Swaps for Better Cholesterol Management
This table offers some straightforward food swaps you can make to reduce your intake of saturated fats and boost heart-healthy nutrients.
| Instead Of This (High Saturated Fat) | Try This (Healthier Alternative) |
|---|---|
| Butter or lard for cooking | Olive oil, rapeseed oil, or avocado oil |
| Full-fat cheese and milk | Reduced-fat dairy options or fortified plant-based milks |
| Crisps and biscuits | A handful of unsalted nuts, seeds, or a piece of fruit |
| Fatty cuts of red meat | Lean protein like chicken, turkey, or oily fish (salmon, tuna) |
| Creamy, rich sauces | Tomato-based sauces, or those made with yoghurt or herbs |
Making these changes consistently can have a real, positive impact on your cholesterol profile without feeling like you're missing out.
Get Moving to Boost the Good Stuff
Physical activity is one of the best tools you have for raising your protective HDL cholesterol—the "good" kind that acts like your body's own cleanup crew. When you exercise, you encourage your body to transport fatty deposits away from your arteries and back to the liver where they can be broken down.
You don't need to sign up for a marathon to reap the rewards. The NHS suggests aiming for at least 150 minutes of moderate-intensity activity each week. That could look like:
- A brisk 30-minute walk on your lunch break, five times a week.
- Getting out on your bike, going for a swim, or even doing some energetic gardening.
- Putting on some music and dancing around the living room.
Health Tip: The most important thing is consistency. Find something you genuinely enjoy, because that’s what you’ll stick with for the long haul. Every little bit of movement counts.
Other Key Lifestyle Habits
Beyond what you eat and how much you move, a few other habits form the foundation of good cholesterol management and overall heart health.
Find Your Healthy Weight: Losing even a small amount of excess weight can make a surprisingly big difference. Dropping just 5-10% of your body weight can significantly lower your LDL and triglyceride levels. It’s all connected; managing your weight often goes hand-in-hand with improving your diet and exercise, creating a powerful positive cycle for your health. This is also a key factor in preventing related conditions; you can learn more about how lifestyle changes can make a difference for metabolic syndrome in our detailed guide.
Quit Smoking for Good: If you smoke, stopping is hands down one of the most impactful things you can do for your heart. Smoking damages the inner lining of your arteries, making them sticky and creating the perfect environment for cholesterol plaque to form. It also actively lowers your protective HDL cholesterol.
Be Mindful of Alcohol: While you might have heard that red wine can be good for the heart, it's a bit more complicated than that. Heavy drinking can send your triglyceride levels and blood pressure soaring. The best approach is to stick to the recommended guidelines of no more than 14 units per week, with several drink-free days in between.
When Lifestyle Changes Aren't Enough

Making positive changes to your diet and getting more active are fantastic first steps in managing your cholesterol. But what happens when you’ve done everything right and your numbers still won’t budge? It can be incredibly frustrating, but it’s definitely not a sign you’ve failed.
More often than not, this points to something you can’t control: your genetics.
For some of us, high cholesterol is simply written into our DNA. Conditions like familial hypercholesterolaemia (FH) mean the body has trouble clearing 'bad' LDL cholesterol from the blood, leading to unusually high levels right from birth. This happens no matter how healthy your lifestyle is.
It’s a crucial reminder that high cholesterol isn't always a direct reflection of your choices. Sometimes, diet and exercise alone just aren't enough to get things into a healthy range.
When Your Doctor May Recommend Medication
If you've committed to healthier habits but your cholesterol remains high, your doctor will likely start a conversation about medication. This is also true if your overall risk of cardiovascular disease is elevated. It’s not a last resort; it’s a proactive and very effective way to protect your long-term heart health.
The go-to medications for high cholesterol are statins. They work by getting straight to the source and reducing how much cholesterol your liver produces. You could think of a statin as a manager telling the body’s main cholesterol factory to slow down its production line.
By making less cholesterol, your liver helps lower the LDL levels floating around in your bloodstream. This dramatically cuts your risk of the artery-clogging plaque that leads to heart attacks and strokes.
Important Advice: Starting medication doesn't mean you can give up on your healthy habits. The two work together as a team. Think of it as a powerful partnership between medicine and your daily choices, giving you the best possible protection. Continue with your diet and exercise plan for optimal results.
When lifestyle adjustments alone aren't quite enough to manage cholesterol and other related health issues, a doctor might also discuss options like prescription weight loss medication.
Ultimately, the goal is to build the strongest possible defence against heart disease. Combining the support of medication with your ongoing commitment to a healthy lifestyle is the most comprehensive strategy for getting your cholesterol under control and securing a healthier future.
Got Questions About Cholesterol? We've Got Answers
It’s easy to get tangled up in the myths and jargon surrounding cholesterol. Getting to grips with the facts is the first step towards taking control of your health. Let’s clear up some of the most common questions we hear.
Can I Have High Cholesterol if I'm Slim and Active?
It’s a common assumption, but the answer is a definite yes. While keeping fit and maintaining a healthy weight are fantastic for your heart, they aren't a guarantee against high cholesterol. The truth is, your genes have a massive say in how your body handles cholesterol.
Some of us are simply wired to produce too much of it, a genetic condition known as familial hypercholesterolaemia. This is precisely why your GP encourages regular checks for everyone—you simply can't tell what your cholesterol levels are just by looking at someone.
Are Eggs Really Bad for My Cholesterol?
This is probably one of the biggest myths out there. For the vast majority of people, the dietary cholesterol you find in foods like eggs has a much smaller effect on your 'bad' LDL cholesterol than the saturated fat in your diet does.
Health Advice: The official UK health advice no longer sets a limit on egg consumption. The real culprit to watch is saturated fat, which you’ll find in things like pastries, fatty cuts of meat, biscuits, and full-fat dairy. Focus on reducing these foods for a bigger impact on your cholesterol.
How Often Should I Get My Cholesterol Checked?
As a rule of thumb, the NHS invites adults in the UK aged 40 to 74 for a Health Check every five years, and that includes a cholesterol test. But think of this as a starting point, not a strict rule.
Your own GP might suggest more frequent checks if you have specific risk factors. These could include:
- A family history of high cholesterol or heart disease.
- Other conditions like diabetes or high blood pressure.
- Lifestyle factors, such as being overweight or a smoker.
The best advice is always personal. Your doctor knows your full health story and can recommend a screening schedule that makes sense for you.
At The Lagom Clinic, we focus on understanding your complete health picture to offer proactive, personalised care. If you'd like to discuss your cholesterol and build a health plan that’s right for you, book a consultation with our private GPs in Bristol today at https://www.thelagom.co.uk.




